This week’s makers are Willis Tang, Nabaan Mir, Paul McMillan Villalobos, Aniket Pratapneni, and Matthew Kim, all students from the School of Medicine. We caught up with them to see what they have been making.
Q: What did you create?
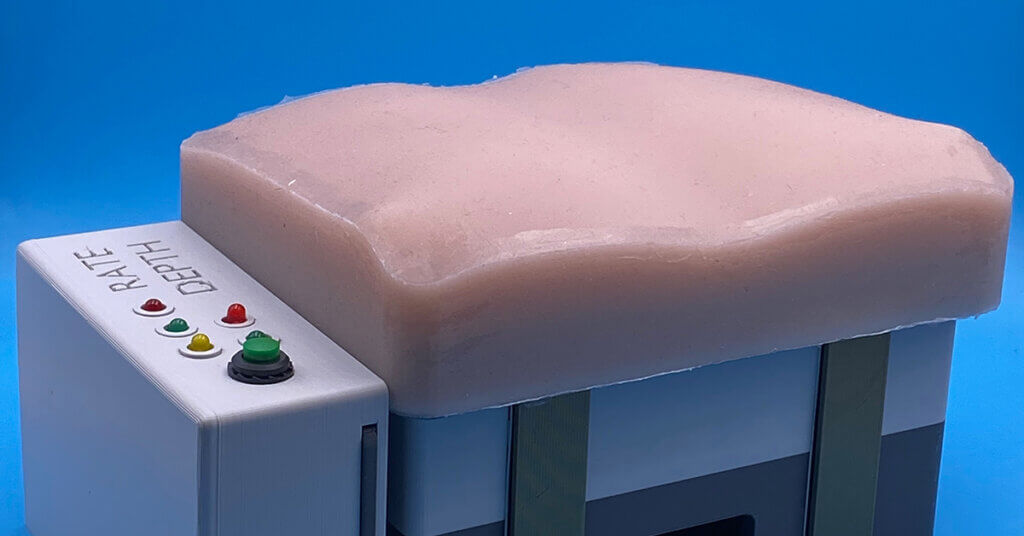
We created a cost-effective, portable cardiopulmonary resuscitation (CPR) training device that provides real-time feedback on compression rate and depth via color-coded, light-emitting diode (LED) lights.
Q: Why did you decide to create it?
Currently available CPR manikins are extremely costly, making them inaccessible to community programs, schools, and learners from low-resource areas. While cheaper alternatives do exist, they are typically made from lower-quality, makeshift materials and lack essential features that teach effective compression techniques. Additionally, many of the current models are quite bulky and difficult to transport. Thus, we sought to create a trainer that retained real-time feedback capabilities while minimizing cost and transport burden.
Q: What was your process like?
We began with a simple concept using springs, plastic housing, and electronic sensors to create a basic prototype. This was followed by numerous iterative stages using Blender, an open-source modeling software, to determine the dimensions and mechanisms of a 3D-printable device. In collaboration with the Makers Lab, we created an evidence-based design measured to match compression depth, rate, and resistance targets reported in existing literature.
For the electronic components, we prototyped the circuitry on a breadboard using an Arduino kit, incorporating LED lights, a buzzer, and an ultrasonic sensor. The software was developed in C++, enabling the system to measure compression depth and calculate compression rate, providing real-time feedback. After testing and finalizing the design, we transitioned to a more compact version, using only the ATmega328P microcontroller and soldered connections on a through-hole perfboard to stabilize the electrical connections and simplify assembly.

Q: What was the most challenging part of the process?
The most challenging part of this process was balancing the variables of cost, size, and functionality. Early in our design stage, we experimented with a significantly smaller, cube-shaped model. We believed it would reduce costs, be easier to transport, and retain much of the same functionality. However, feedback from physicians noted that the reduced surface area compromised proper CPR hand positioning. Based on this feedback, we returned to a larger design and added a thin silicone layer modeled after chest anatomy to improve touchable realism while maintaining manageable size and affordability.

Q: What was your favorite part of the process?
Our favorite part of the process was seeing all the different components of our project come together. We initially began with a piece of plastic and some springs, but ended up with a fully responsive model that has been piloted in several CPR training sessions in the United States and at various international institutions.

Q: How has this project contributed to your education?
This project gave us hands-on experience engaging with the full lifecycle of creating a medical device. This included identifying a need, to prototyping, testing, and refining a functional tool. We also developed practical skills in 3D modeling, circuitry, embedded programming, and iterative design. Furthermore we learned how to incorporate critical user feedback from clinicians and instructors.
Q: What do you plan to create next?
We plan to continue reducing production costs and adding new features. We are currently working on the next iteration, which includes a more compact electronics module, expanded data collection, and export capabilities. These features support research and allow instructors to track learner performance.